 Iliotibial Band Syndrome (ITBS) is a common knee injury in runners and cyclists that usually presents as lateral (outer) knee pain caused by inflammation of the distal (bottom) portion of the iliotibial band. In some cases, the iliotibial band becomes inflamed at its proximal (upper) origin and causes referred hip pain.
Iliotibial Band Syndrome (ITBS) is a common knee injury in runners and cyclists that usually presents as lateral (outer) knee pain caused by inflammation of the distal (bottom) portion of the iliotibial band. In some cases, the iliotibial band becomes inflamed at its proximal (upper) origin and causes referred hip pain.
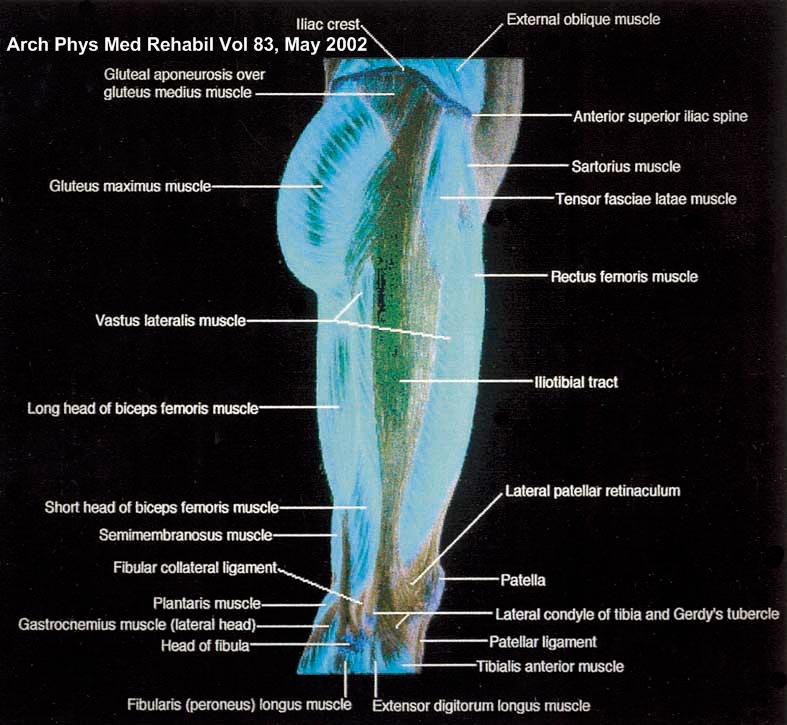
The iliotibial band (ITB) is a thickening of the lateral (outer) soft tissue that envelopes the leg muscle. The thickened tissue is known as fascia and in this area of the upper leg it is called the fascia lata. The ITB starts near the anterior superior iliac spine ( front of pelvis) and inserts into Gerdy’s tubercle on the tibia.
The ITB is considered a continuation of the tendinous portion of the tensor fascia lata muscle and is indirectly attached to parts of the gluteus medius, gluteus maximus, and the vastus lateralis muscles. Distally, the ITB spans out and inserts on the lateral border of the patella, the lateral patellar retinaculum, and Gerdy’s tubercle of the tibia.
Causes
ITBS is caused by a combination of overuse and biomechanical factors.
- Hip abductor muscle weakness and imbalance.
- Sudden increase in mileage.
- Increase in track or interval training.
- Crowned running surface.
- Tight iliotibial band.
- Excessive foot pronation
Treatment protocol
 ITBS can be extremely challenging to treat. Treatment requires active patient participation and compliance with activity modification.
ITBS can be extremely challenging to treat. Treatment requires active patient participation and compliance with activity modification.
- Strengthening the hip abductors and stretching the ITB and the structures that attach in to it are usually the keys to recovering from this problem.
- A study by Fredericson published in the Archives of Physical medicine suggests that adding an overhead arm extension to the most common lateral ITB stretch increases average ITB length change and average external adduction moments in male elite-level distance runners.
- Altering training regimens.
- Temporary decrease or stopping training
- Avoid crowned surfaces or too much running around a track
- Shorten your stride
- Wear motion control shoes to limit pronation or If you have been wearing motion control shoes, change to a less controlling shoe.
- Foot orthotics
- Corticosteroid injections
- Surgical release of the iliotibial band.
If your ilio tibial band syndrome does not resolve after a stretching and strengthening treatment protocol you may have to consider there may be another problem causing this lateral knee and thigh pain. The alternate diagnoses for lateral knee pain is as follows:
- Lateral meniscal tear
- Lateral collateral ligament sprain
- Biceps femoris tendinopathy
- Patellofemoral pain syndrome
- Lateral patellar compression syndrome
- Popliteal tendinopathy
- Stress reaction or stress fracture
- Proximal tibial-fibular joint sprain
- Referred pain from lumbar spine
- Referred pain from peroneal nerve injury
