Bunion (Hallux Valgus) Treatment in Whitby
A bunion is a bony bump that forms at the base of the big toe when the joint becomes misaligned. As the big toe drifts toward the second toe, the joint becomes prominent, irritated, and painful—especially in tight or narrow shoes. We assess and treat bunions at our Whitby clinic to help reduce pain, improve comfort, and slow progression.
What Is a Bunion?
A bunion (hallux valgus) occurs when the big toe angles inward toward the second toe. This shift causes the joint at the base of the big toe to protrude outward, creating a visible bump. Over time, the deformity can worsen, leading to increased pain, difficulty fitting shoes, and changes in how you walk.
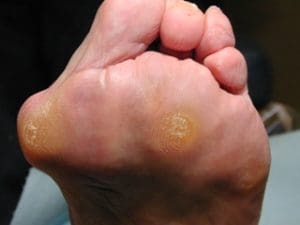
Why Bunions Develop
Bunions form when abnormal pressure and stress cause the big toe joint to become unstable. Contributing factors include:
-
Inherited foot structure
-
Flat feet or hypermobility
-
Foot injuries
-
Arthritis
-
Tight or narrow footwear
-
Occupations requiring prolonged standing

Symptoms of Bunions
-
A visible bump at the base of the big toe
-
Swelling, redness, or soreness
-
Calluses along the inside edge of the toe
-
Corns or calluses under the ball of the foot
-
Persistent or intermittent pain
-
Restricted movement of the big toe
How Bunions Progress
Without treatment, bunions can gradually worsen. The big toe may continue to drift, the bump may enlarge, and pain may increase. Secondary problems such as hammertoes, corns, calluses, and metatarsalgia may develop due to altered foot mechanics.
Assessment
A chiropodist or family doctor can identify a bunion through:
-
Physical exam
-
Range‑of‑motion testing
-
Assessment of redness, swelling, and pain
-
X‑rays to evaluate joint angles and arthritis
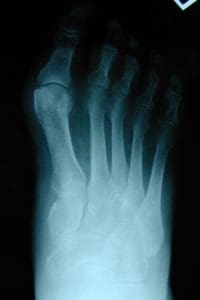
Your content goes here. Edit or remove this text inline or in the module Content settings. You can also style every aspect of this content in the module Design settings and even apply custom CSS to this text in the module Advanced settings.
Bunion Treatment in Whitby
We provide full assessment, footwear guidance, orthotic therapy, and conservative management for bunions. When needed, we refer for surgical consultation.
Treatment Options for Bunions
Footwear Changes
Wearing shoes with a wide, deep toe box reduces pressure on the bunion and helps relieve pain.
Padding and Protection
Non‑medicated bunion pads can reduce friction and irritation.
Orthotics
Custom orthotics help correct abnormal foot mechanics, reduce pressure on the bunion, and slow progression.
Manual Therapy
Mobilizing stiff joints can improve comfort and function.
Medication
Over‑the‑counter pain relievers (acetaminophen, ibuprofen, naproxen) may help reduce discomfort.
Corticosteroid Injections
Used for significant inflammation or joint irritation.
Surgery
If conservative treatment fails or the deformity becomes severe, surgery may be recommended to realign the joint. Recovery varies depending on the procedure.
When to Seek Treatment
Book an assessment if you experience:
-
Persistent pain in the big toe joint
-
Difficulty wearing shoes
-
A bunion that is getting larger
-
Second‑toe crowding or deformity
-
Pain under the ball of the foot
-
Limited movement of the big toe
Early treatment can slow progression and reduce long‑term complications.
Bunion Treatment in Whitby
We provide full assessment, footwear guidance, orthotic therapy, and conservative management for bunions. When needed, we refer for surgical consultation. Our goal is to reduce pain, improve comfort, and help you stay active.
Book an Appointment
Book an appointment, if you’re experiencing bunion pain or difficulty wearing shoes, we can help. Our chiropodists assess foot structure, joint alignment, and gait mechanics to create a personalized treatment plan.
